FluView Summary ending on February 19, 2022
Updated February 25, 2022

Note: CDC is tracking the COVID-19 pandemic in a weekly publication called COVID Data Tracker Weekly Review.
All data are preliminary and may change as more reports are received.
A description of the CDC influenza surveillance system, including methodology and detailed descriptions of each data component is available on the surveillance methods page.
Additional information on the current and previous influenza seasons for each surveillance component are available on FluView Interactive.
Sporadic influenza activity continues across the country. In some areas, influenza activity is increasing.
Viruses
Severe Disease
All data are preliminary and may change as more reports are received.
A description of the CDC influenza surveillance system, including methodology and detailed descriptions of each data component is available on the surveillance methods page.
Additional information on the current and previous influenza seasons for each surveillance component are available on FluView Interactive.
Key Points
- Sporadic influenza activity continues across the country. In some areas, influenza activity is increasing.
- The majority of influenza viruses detected are A(H3N2). H3N2 viruses identified so far this season are genetically closely related to the vaccine virus. Antigenic data, now included in FluView, show that the majority of the H3N2 viruses characterized are antigenically different from the vaccine reference viruses. While the number of B/Victoria viruses circulating this season is small, the majority of the B/Victoria viruses characterized are antigenically similar to the vaccine reference virus.
- The percentage of outpatient visits due to respiratory illness remained stable nationally compared to last week and is below baseline. Influenza is contributing to levels of respiratory illness, but other respiratory viruses are also circulating. The relative contribution of influenza varies by location.
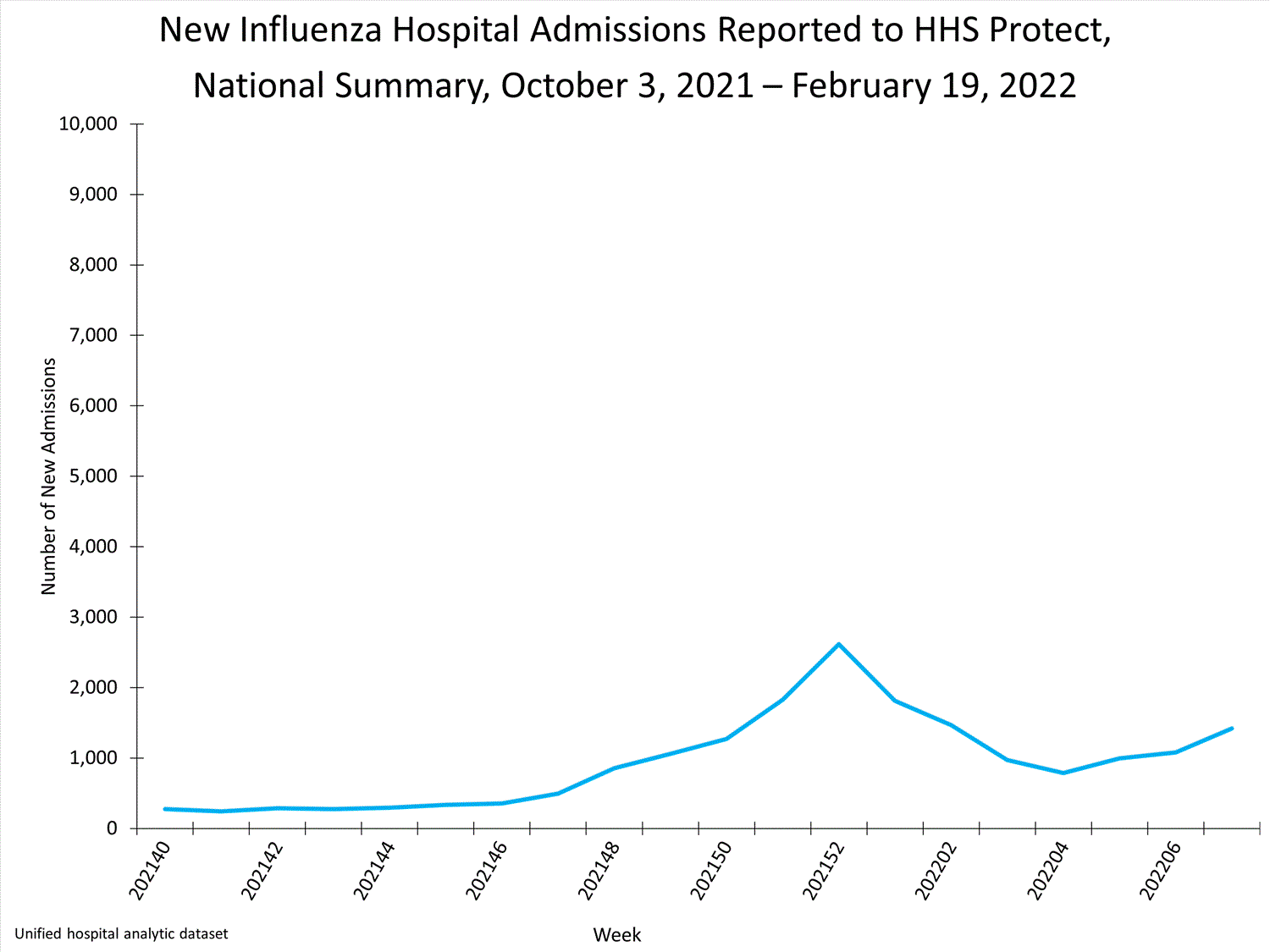
- The number of hospital admissions reported to HHS Protect has increased for the past three weeks.
- The cumulative hospitalization rate in the FluSurv-NET system is higher than the rate for the entire 2020-2021 season, but lower than the rate seen at this time during the four seasons preceding the COVID-19 pandemic.
- One influenza-associated pediatric death was reported this week. This is the sixth pediatric death reported this season.
- CDC estimates that so far this season there have been at least 2.4 million flu illnesses, 23,000 hospitalizations, and 1,400 deaths from flu.
- An annual flu vaccine is the best way to protect against flu and its potentially serious complications. CDC continues to recommend that everyone ages 6 months and older get a flu vaccine as long as flu activity continues.
- Flu vaccination coverage remains lower this season compared to last.
- Flu vaccines are available at many different locations, including pharmacies and health departments. Visit www.vaccines.gov to find a flu vaccine near you.
- There are also flu antiviral drugs that can be used to treat flu illness.
U.S. Virologic Surveillance
Influenza A(H3N2) viruses have been the most frequently detected influenza viruses this season. Of the 7,560 influenza positives reported this season by the public health labs and also tested for SARS-CoV-2, 456 (6.0%) were also positive for SARS-CoV-2. For regional and state level data and age group distribution, please visit FluView Interactive. Viruses known to be associated with recent live attenuated influenza vaccine (LAIV) receipt or found upon further testing to be a vaccine virus are not included as they are not circulating influenza viruses.
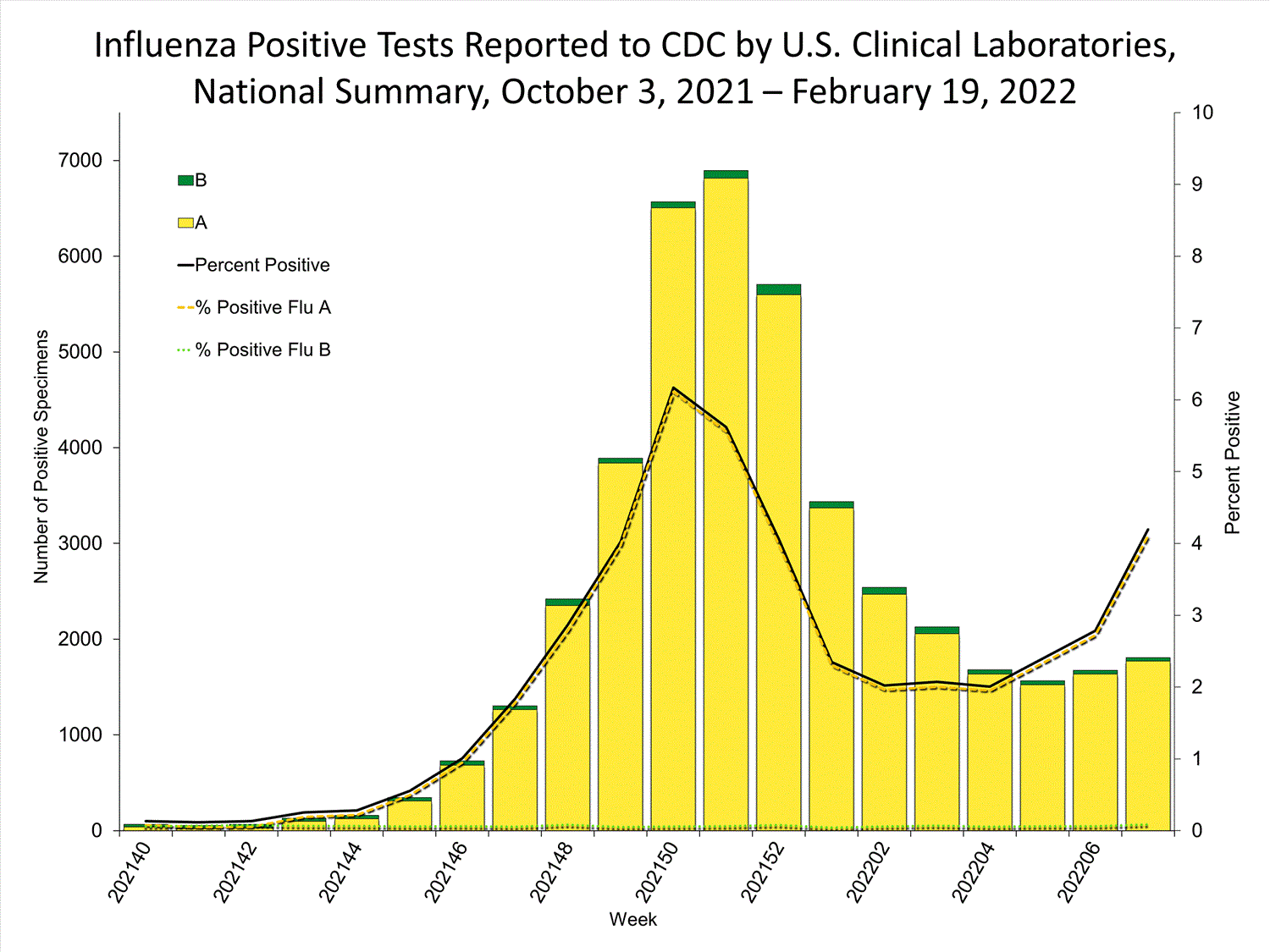
Clinical Laboratories
The results of tests performed by clinical laboratories nationwide are summarized below. Data from clinical laboratories (the percentage of specimens tested that are positive for influenza) are used to monitor whether influenza activity is increasing or decreasing.
| Week 7 | Data Cumulative since October 3, 2021 (Week 40) |
|
|---|---|---|
| No. of specimens tested | 43,078 | 1,634,117 |
| No. of positive specimens (%) | 1,807 (4.2%) | 43,153 (2.6%) |
| Positive specimens by type | ||
| Influenza A | 1,770 (98.0%) | 42,137 (97.6%) |
| Influenza B | 37 (2.0%) | 1,016 (2.4%) |
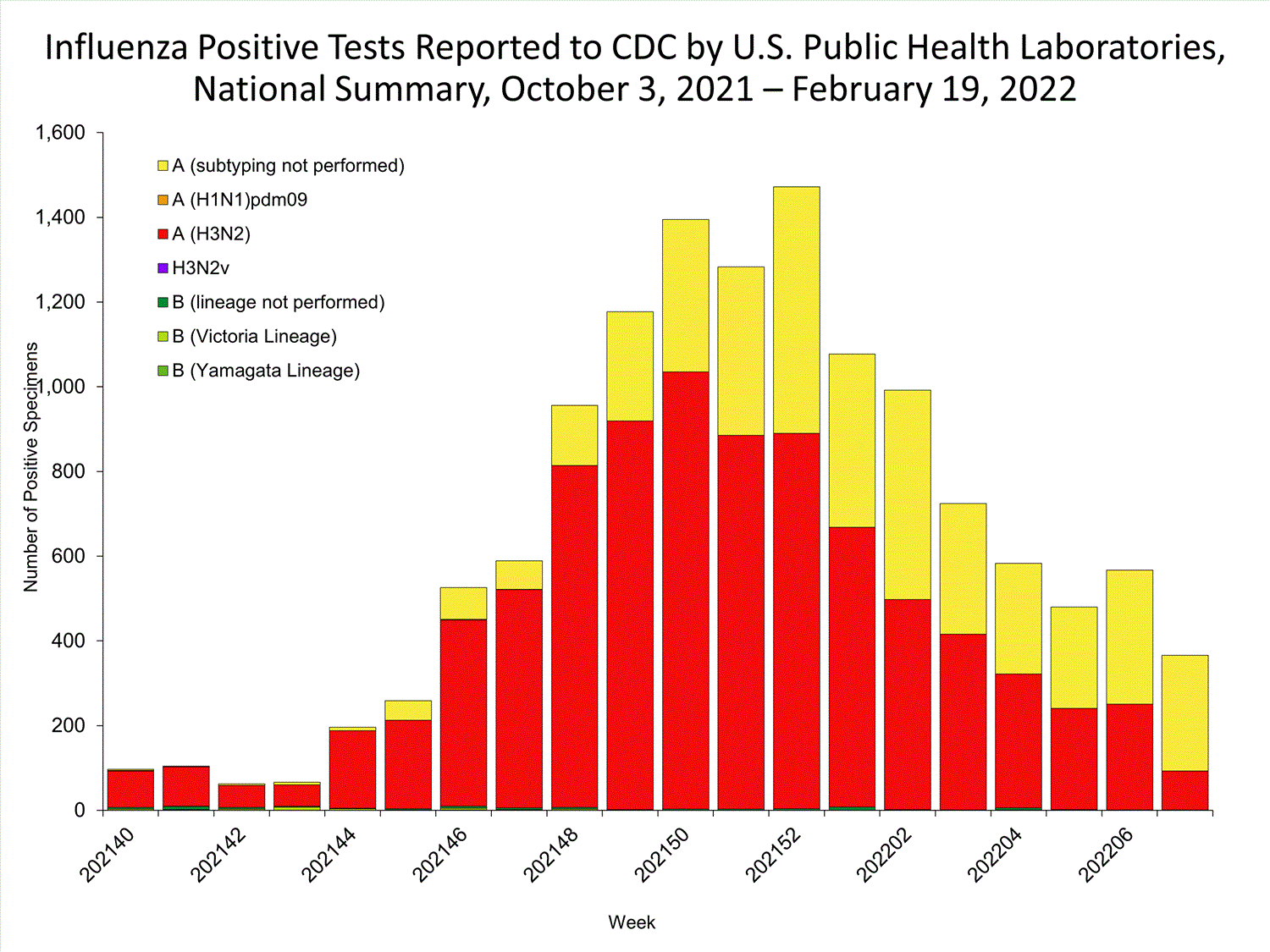
Public Health Laboratories
The results of tests performed by public health laboratories nationwide are summarized below. Data from public health laboratories are used to monitor the proportion of circulating viruses that belong to each influenza subtype/lineage.
| Week 7 | Data Cumulative since October 3, 2021 (Week 40) |
|
|---|---|---|
| No. of specimens tested | 18,582 | 632,699 |
| No. of positive specimens | 366 | 12,971 |
| Positive specimens by type/subtype | ||
| Influenza A | 365 (99.7%) | 12,873 (99.2%) |
| (H1N1)pdm09 | 0 | 4 (<0.1%) |
| H3N2 | 92 (100%) | 8,619 (99.9%) |
| H3N2v | 0 | 1 (<0.1%) |
| Subtyping not performed | 273 | 4,249 |
| Influenza B | 1 (0.3%) | 98 (0.8%) |
| Yamagata lineage | 0 | 1 (2.9%) |
| Victoria lineage | 0 | 33 (97.1%) |
| Lineage not performed | 1 | 64 |
Additional virologic surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive: National, Regional, and State Data or Age Data
Influenza Virus Characterization
CDC performs genetic and antigenic characterization of U.S. viruses submitted from state and local public health laboratories using the Right Size Roadmap submission guidance. These data are used to compare how similar the currently circulating influenza viruses are to the reference viruses representing viruses contained in the current influenza vaccines. The data are also used to monitor evolutionary changes that continually occur in influenza viruses circulating in humans. CDC also tests susceptibility of circulating influenza viruses to antiviral medications including the neuraminidase inhibitors (oseltamivir, zanamivir, and peramivir) and the PA endonuclease inhibitor baloxavir.
CDC has genetically characterized 641 influenza viruses collected since October 3, 2021. H3N2 viruses identified so far this season are genetically closely related to the vaccine virus, but there are some antigenic differences that have developed as H3N2 viruses have continued to evolve.
| Virus Subtype or Lineage | Genetic Characterization | ||||
|---|---|---|---|---|---|
| Total No. of Subtype/Lineage Tested |
HA Clade |
Number (% of subtype/lineage tested) |
HA Subclade |
Number (% of subtype/lineage tested) |
|
| A/H1 | 3 | ||||
| 6B.1A | 3 (100%) | 5a.1 | 2 (66.7%) | ||
| 5a.2 | 1 (33.3%) | ||||
| A/H3 | 618 | ||||
| 3C.2a1b | 618 (100%) | 1a | 1 (0.1%) | ||
| 1b | 1 (0.1%) | ||||
| 2a | 0 | ||||
| 2a.1 | 0 | ||||
| 2a.2 | 616 (99.8%) | ||||
| 3C.3a | 0 | 3a | 0 | ||
| B/Victoria | 20 | ||||
| V1A | 20 (100%) | V1A | 0 | ||
| V1A.1 | 0 | ||||
| V1A.3 | 9 (45.0%) | ||||
| V1A.3a | 0 | ||||
| V1A.3a.1 | 0 | ||||
| V1A.3a.2 | 11 (55.0%) | ||||
| B/Yamagata | 0 | ||||
| Y3 | 0 | ||||
CDC antigenically characterizes influenza viruses by hemagglutination inhibition (HI) (H1N1pdm09, B/Victoria and B/Yamagata viruses) or neutralization-based HINT (H3N2 viruses) using antisera that ferrets make after being infected with reference viruses representing the 2021-2022 Northern Hemisphere recommended egg-based and cell or recombinant-based vaccine viruses. Antigenic differences between viruses are determined by comparing how well the antibodies made against the vaccine reference viruses recognize the circulating viruses that have been grown in cell culture. Ferret antisera are useful because antibodies raised against a particular virus can often recognize small changes in the surface proteins of other viruses. In HI assays, viruses with similar antigenic properties have antibody titer differences of less than or equal to 4-fold when compared to the reference (vaccine) virus. In HINT, viruses with similar antigenic properties have antibody neutralization titer differences of less than 8-fold. Viruses selected for antigenic characterization are a subset representing the genetic changes in the surface proteins seen in genetically characterized viruses.
Influenza A Viruses
- A (H1N1)pdm09: Two A(H1N1)pdm09 viruses were antigenically characterized by HI, and 1 (50%) was well recognized (reacting at titers that were within 4-fold of the homologous virus titer) by ferret antisera to cell-grown A/Wisconsin/588/2019-like reference viruses representing the A(H1N1)pdm09 component for the cell- and recombinant-based influenza vaccines and 1 (50%) was well recognized by ferret antisera to egg-grown A/Victoria/2570/2019-like reference viruses representing the A(H1N1)pdm09 component for the egg-based influenza vaccines.
- A (H3N2): A subset of fifty-eight A(H3N2) viruses were antigenically characterized by HINT, and 2 (3%) were well recognized (reacting at titers that were within 8-fold of the homologous virus titer) by ferret antisera to cell-grown A/Cambodia/E0826360/2020-like reference viruses representing the A(H3N2) component for the cell- and recombinant-based influenza vaccines and 18 (31%) were well recognized by ferret antisera to egg-grown A/Cambodia/E0826360/2020-like reference viruses representing the A(H3N2) component for egg-based influenza vaccines.
Influenza B Viruses
- B/Victoria: Thirteen B/Victoria lineage viruses were antigenically characterized by HI, and 11 (85%) were well recognized (reacting at titers that were within 4-fold of the homologous virus titer) by ferret antisera to cell-grown B/Washington/02/2019-like reference viruses representing the B/Victoria component for the cell- and recombinant-based influenza vaccines and 11 (85%) were well recognized by ferret antisera to egg-grown B/Washington/02/2019-like reference viruses representing the B/Victoria component for egg-based influenza vaccines.
- B/Yamagata: No influenza B/Yamagata-lineage viruses were available for antigenic characterization.
Assessment of Virus Susceptibility to Antiviral Medications
CDC assesses susceptibility of influenza viruses to antiviral medications including the neuraminidase inhibitors (oseltamivir, zanamivir, and peramivir) and the PA endonuclease inhibitor baloxavir using next generation sequence analysis supplemented by laboratory assays. Information about antiviral susceptibility test methods can be found at U.S. Influenza Surveillance: Purpose and Methods | CDC.
Viruses collected in the United States since October 3, 2021, were tested for antiviral susceptibility as follows:
| Antiviral Medication | Total Viruses |
A/H1 | A/H3 | B/Victoria | B/Yamagata | ||
|---|---|---|---|---|---|---|---|
| Neuraminidase Inhibitors |
|||||||
| Oseltamivir | Viruses Tested |
658 | 3 | 635 | 20 | 0 | |
| Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| Highly Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| Peramivir | Viruses Tested |
658 | 3 | 635 | 20 | 0 | |
| Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| Highly Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| Zanamivir | Viruses Tested |
658 | 3 | 635 | 20 | 0 | |
| Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| Highly Reduced Inhibition |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
| PA Cap-Dependent Endonuclease Inhibitor | Baloxavir | Viruses Tested |
650 | 3 | 627 | 20 | 0 |
| Reduced Susceptibility |
(0.0%) | (0.0%) | (0.0%) | (0.0%) | (0.0%) | ||
High levels of resistance to the adamantanes (amantadine and rimantadine) persist among influenza A(H1N1)pdm09 and influenza A(H3N2) viruses (the adamantanes are not effective against influenza B viruses). Therefore, use of these antivirals for treatment and prevention of influenza A virus infection is not recommended and data from adamantane resistance testing are not presented.
Outpatient Respiratory Illness Surveillance
The U.S. Outpatient Influenza-like Illness Surveillance Network (ILINet) monitors outpatient visits for influenza-like illness [ILI (fever plus cough or sore throat)], not laboratory-confirmed influenza, and will therefore capture respiratory illness visits due to infection with any pathogen that can present with similar symptoms, including influenza, SARS-CoV-2, and RSV. Due to the COVID-19 pandemic, health care-seeking behaviors have changed, and people may be accessing the health care system in alternative settings not captured as a part of ILINet or at a different point in their illness than they might have before the pandemic. Therefore, it is important to evaluate syndromic surveillance data, including that from ILINet, in the context of other sources of surveillance data to obtain a complete and accurate picture of influenza, SARS-CoV-2, and other respiratory virus activity. CDC is tracking the COVID-19 pandemic in a weekly publication called COVID Data Tracker Weekly Review. Information about other respiratory virus activity can be found on CDC’s National Respiratory and Enteric Virus Surveillance System (NREVSS) website.
Outpatient Respiratory Illness Visits
Nationwide during week 7, 1.5% of patient visits reported through ILINet were due to respiratory illness that included fever plus a cough or sore throat, also referred to as ILI. This percentage is below the national baseline. All 10 HHS regions are below their region-specific baselines. Multiple respiratory viruses are co-circulating, and the relative contribution of influenza virus infection to ILI varies by location.
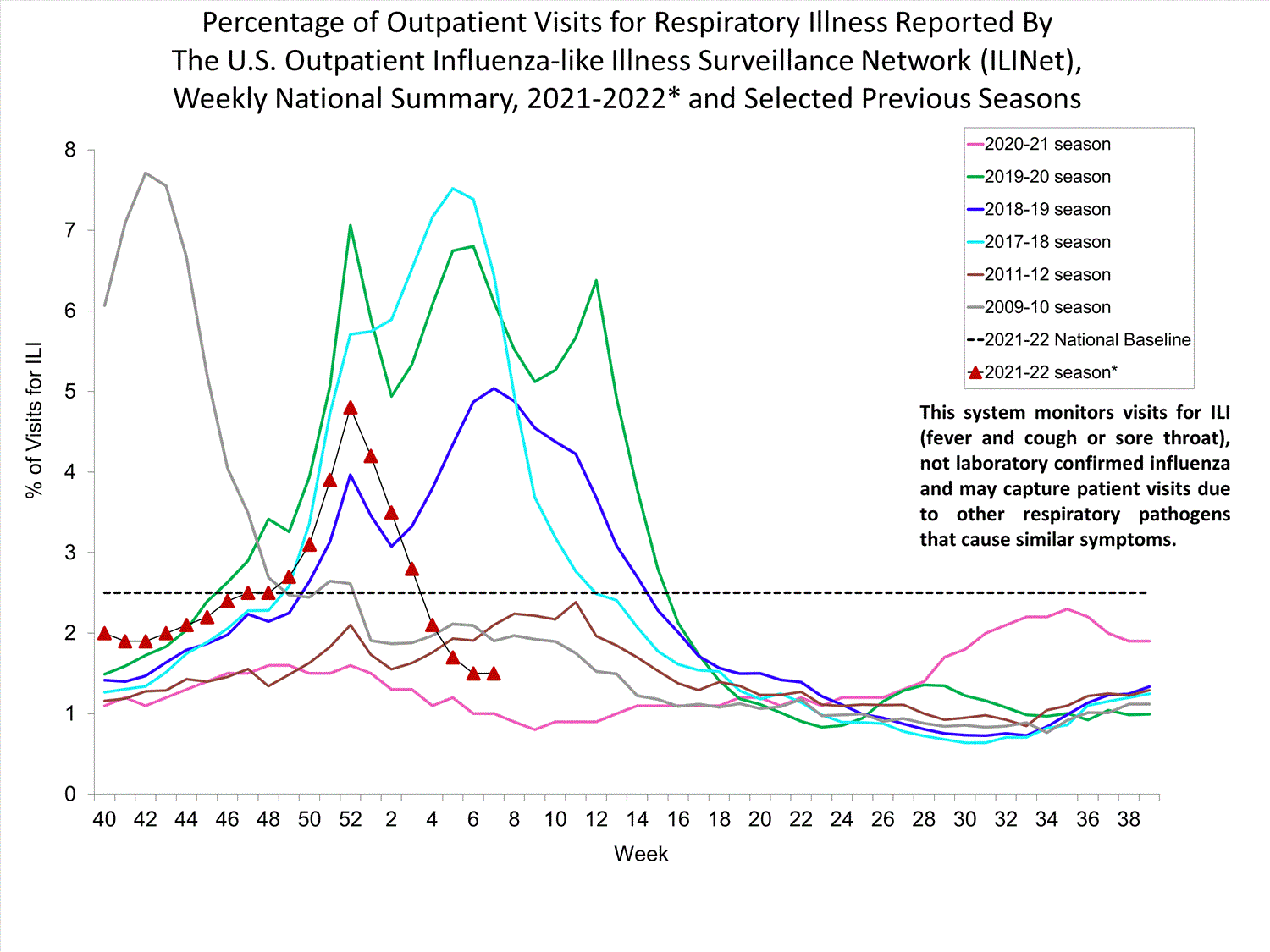
* Effective October 3, 2021 (week 40), the ILI definition (fever plus cough or sore throat) no longer includes “without a known cause other than influenza.”
Outpatient Respiratory Illness Visits by Age Group
More than 70% of ILINet participants provide both the number of patient visits for respiratory illness and the total number of patient visits for the week broken out by age group. Data from this subset of providers are used to calculate the percentages of patient visits for respiratory illness by age group.
The percentage of visits for respiratory illness reported in ILINet in week 7 increased among one age group (5–24 years) compared to week 6. The percentage of visits for respiratory illness in the other age groups (0–4 years, 25-49 years, 50–64 years, and 65+ years) continues to trend downwards.
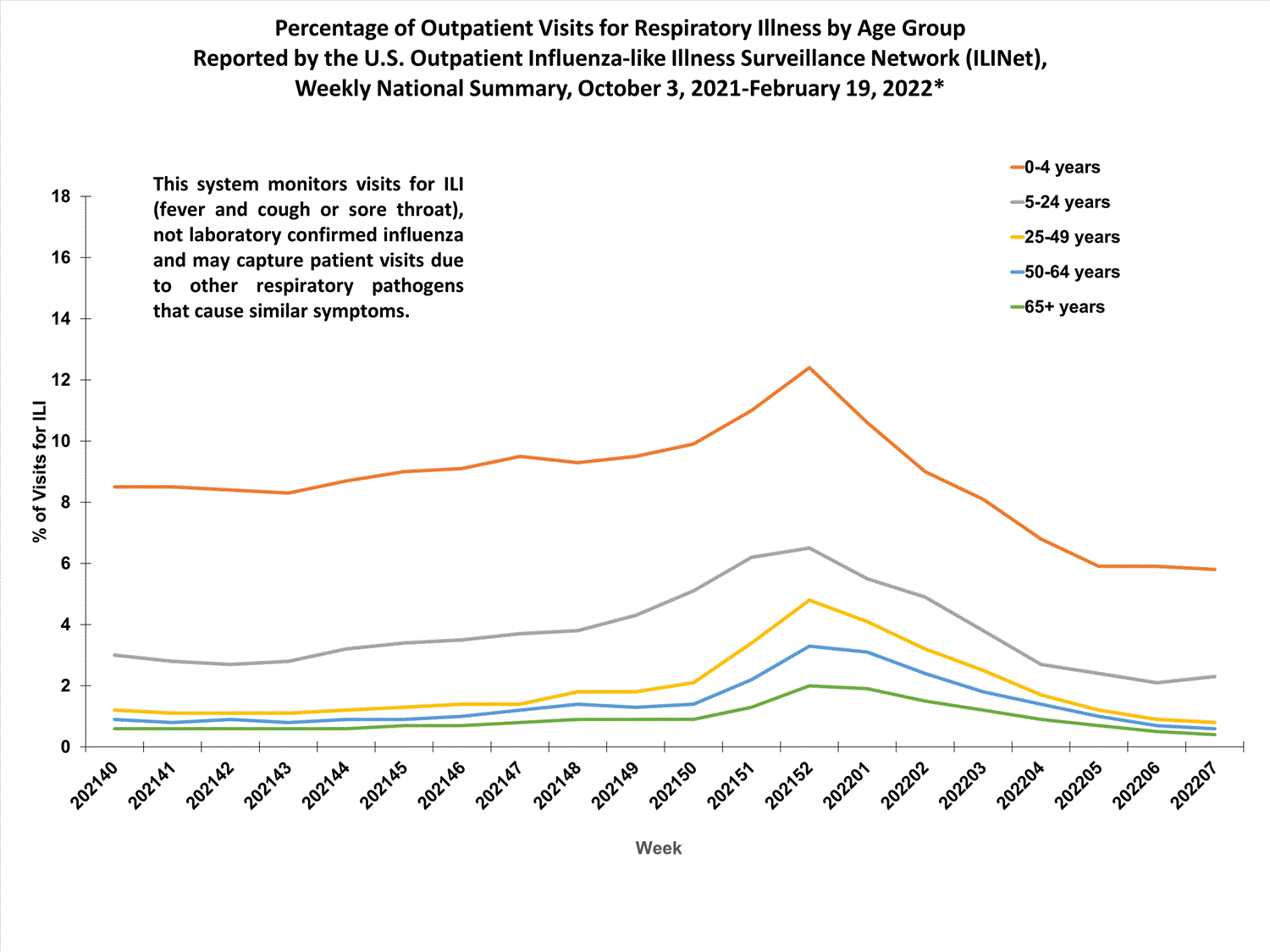
* Effective October 3, 2021 (week 40), the ILI definition (fever plus cough or sore throat) no longer includes “without a known cause other than influenza.”
Outpatient Respiratory Illness Activity Map
Data collected in ILINet are used to produce a measure of ILI activity* by state/jurisdiction and Core Based Statistical Areas (CBSA).
| Activity Level | Number of Jurisdictions | Number of CBSAs | ||
|---|---|---|---|---|
| Week 7
(Week ending |
Week 6
(Week ending |
Week 7
(Week ending |
Week 6
(Week ending |
|
| Very High | 0 | 0 | 4 | 4 |
| High | 0 | 0 | 1 | 2 |
| Moderate | 2 | 0 | 17 | 10 |
| Low | 3 | 8 | 40 | 52 |
| Minimal | 48 | 46 | 594 | 602 |
| Insufficient Data | 2 | 1 | 273 | 259 |
*Data collected in ILINet may disproportionally represent certain populations within a jurisdiction or CBSA, and therefore, may not accurately depict the full picture of influenza activity for the entire jurisdiction or CBSA. Differences in the data presented here by CDC and independently by some health departments likely represent differing levels of data completeness with data presented by the health department likely being the more complete.
Additional information about medically attended visits for ILI for current and past seasons:
Surveillance Methods | FluView Interactive: National, Regional, and State Data or ILI Activity Map
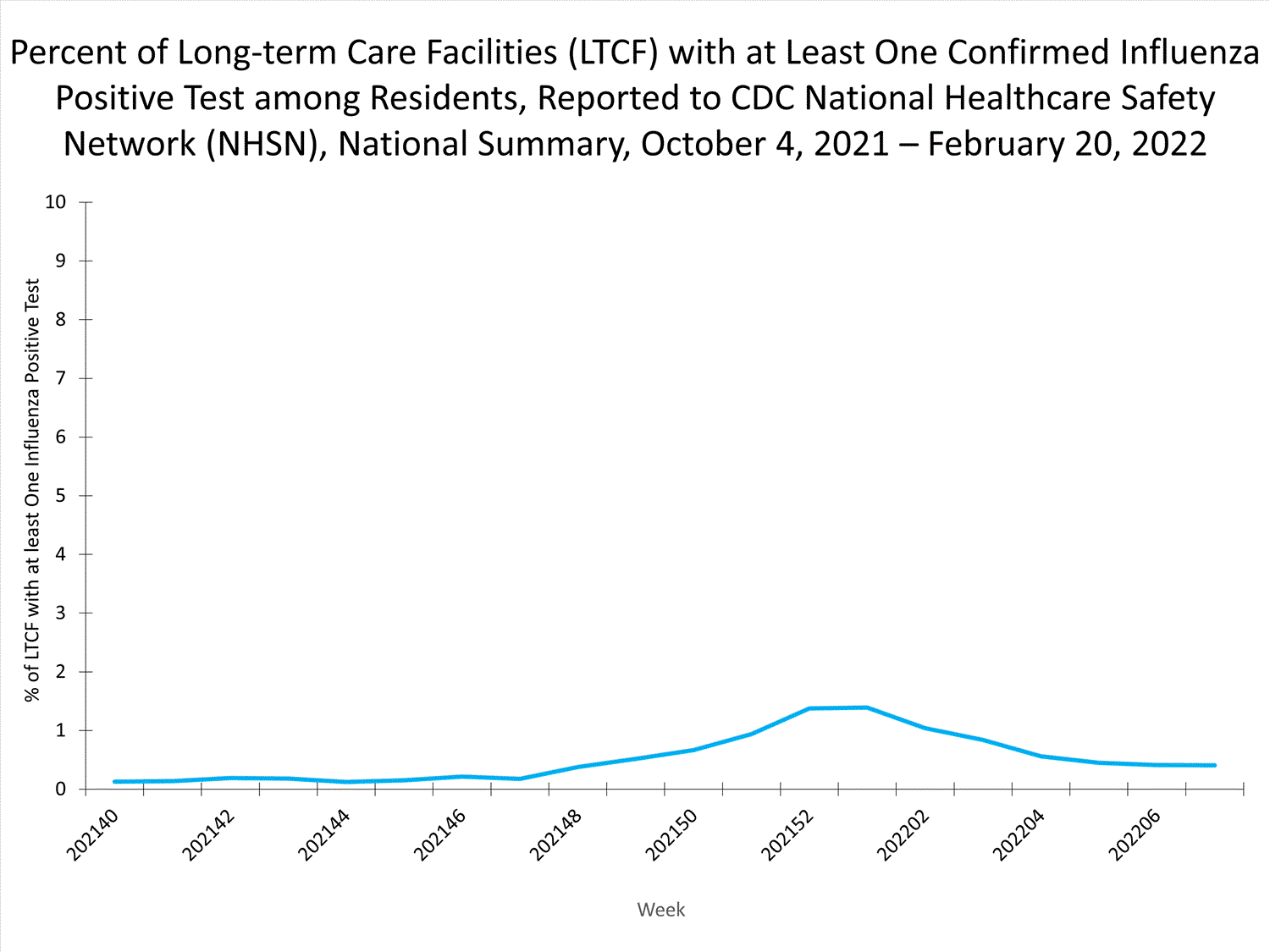
Long-term Care Facility (LTCF) Surveillance
LTCFs (e.g., nursing homes/skilled nursing, long-term care for the developmentally disabled, and assisted living facilities) from all 50 states and U.S. territories report data on influenza virus infections among residents through the National Healthcare Safety Network (NHSN) Long-term Care Facility Component. During week 7, 58 (0.4%) of 14,243 reporting LTCFs reported at least one influenza positive test among their residents.
Additional information about long-term care facility surveillance:
Surveillance Methods | Additional Data
Hospitalization Surveillance
FluSurv-NET
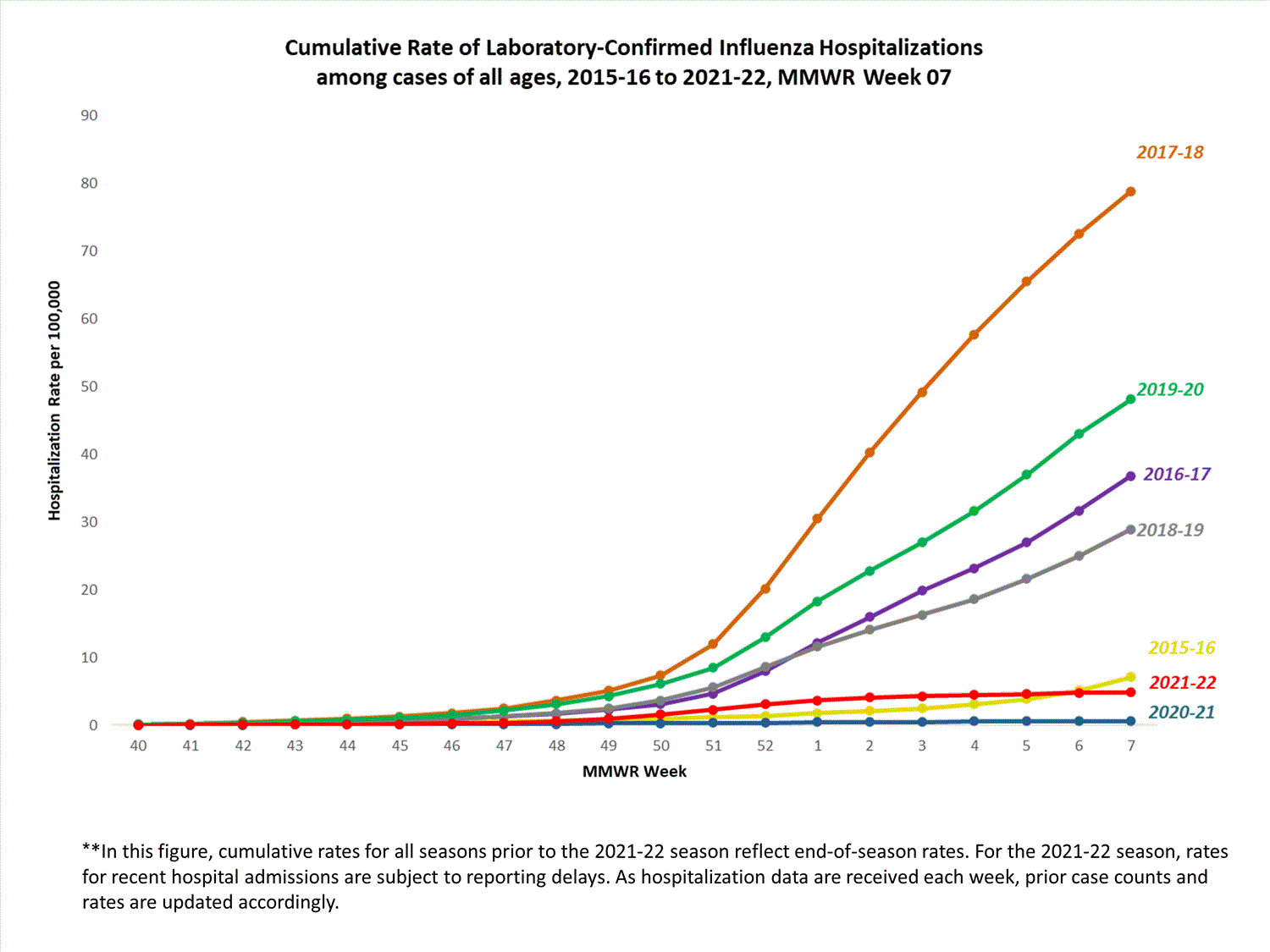
The Influenza Hospitalization Surveillance Network (FluSurv-NET) conducts population-based surveillance for laboratory-confirmed influenza-related hospitalizations in select counties in 14 states and represents approximately 9% of the U.S. population. FluSurv-NET hospitalization data are preliminary. As data are received each week, prior case counts and rates are updated accordingly.
A total of 1,441 laboratory-confirmed influenza-associated hospitalizations were reported by FluSurv-NET sites between October 1, 2021, and February 19, 2022. The overall cumulative hospitalization rate was 4.9 per 100,000 population. This cumulative hospitalization rate is higher than the cumulative in-season hospitalization rate observed in week 7 during the 2020-2021 season (0.6 per 100,000), but lower than the in-season rates observed in week 7 during the 4 seasons preceding the COVID-19 pandemic (these ranged from 27.4 to 74.5 per 100,000 during the 2016-17 through 2019-20 seasons).
When examining rates by age, the highest rate of hospitalization per 100,000 population was among adults aged 65 and older (12.9). Among adults aged ≥65 years, rates were highest among adults aged ≥85 (27.3). Among persons aged <65 years, hospitalization rates per 100,000 population were highest among children aged 0-4 years (7.1) followed by adults aged 50-64 years (4.7). When examining rates by race and ethnicity, the highest rate of hospitalization per 100,000 population was among non-Hispanic American Indian or Alaska Native persons (6.4), followed by non-Hispanic Black persons (6.2).
Among 1,441 hospitalizations, 1,358 (94.2%) were associated with influenza A virus, 76 (5.3%) with influenza B virus, 4 (0.3%) with influenza A virus and influenza B virus co-infection, and 3 (0.2%) with influenza virus for which the type was not determined. Among 353 hospitalizations with influenza A subtype information, 349 (98.9%) were A(H3N2), and 4 (1.1%) were A(H1N1)pdm09. Based on preliminary data, of the 1,441 laboratory-confirmed influenza-associated hospitalizations, 3.5% also tested positive for SARS-CoV-2.
Among 713 hospitalized adults with information on underlying medical conditions, 90% had at least one reported underlying medical condition, the most commonly reported were hypertension, cardiovascular disease, metabolic disorder, and obesity. Among 62 hospitalized children with information on underlying medical conditions, 69.4% had at least one reported underlying medical condition; the most commonly reported condition was asthma.
Additional FluSurv-NET hospitalization surveillance information for current and past seasons and additional age groups:
Surveillance Methods |FluView Interactive: Rates by Age, Sex, and Race/Ethnicity or Data on Patient Characteristics
FluSurv-Net data are used to generate national estimates of the total numbers of influenza cases, medical visits, hospitalizations, and deaths. This season, CDC is reporting preliminary cumulative in-season estimates, which are available at https://www.cdc.gov/flu/about/burden/preliminary-in-season-estimates.htm
HHS-Protect Hospitalization Surveillance
Hospitals report to HHS-Protect the number of patients admitted with laboratory-confirmed influenza. During week 7, 1,420 patients with laboratory-confirmed influenza were admitted to the hospital.
Effective February 2, 2022, hospitals are required to report laboratory-confirmed influenza hospitalizations to HHS-Protect daily. Prior to this update, reporting influenza hospitalizations was optional. See COVID-19 Guidance for Hospital Reporting and FAQs for additional details on this guidance.
Additional HHS Protect hospitalization surveillance information:
Surveillance Methods | Additional Data
Mortality Surveillance
National Center for Health Statistics (NCHS) Mortality Surveillance
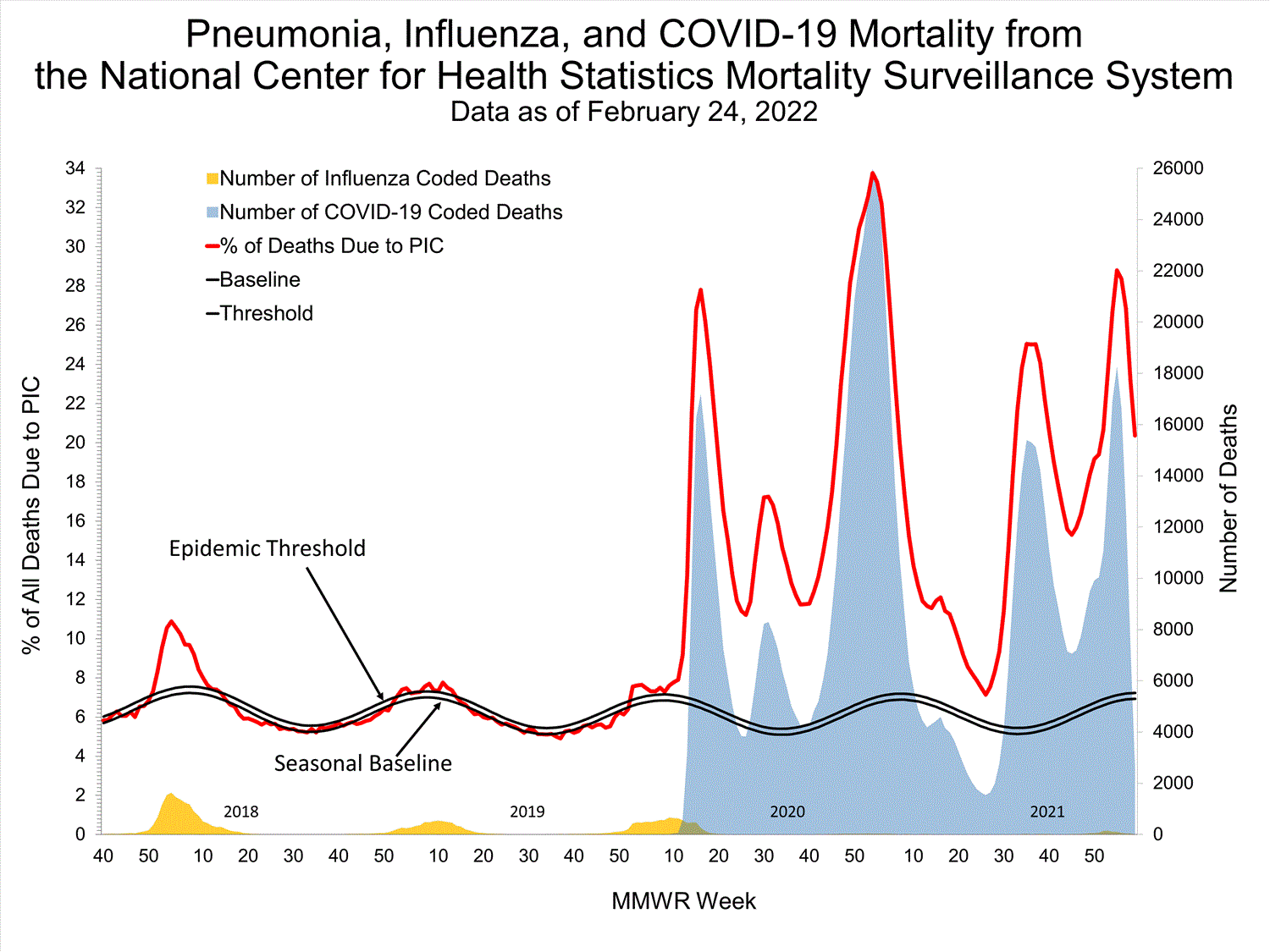
Based on NCHS mortality surveillance data available on February 24, 2022, 20.4% of the deaths that occurred during the week ending February 19, 2022 (week 7), were due to pneumonia, influenza, and/or COVID-19 (PIC). This percentage is above the epidemic threshold of 7.2% for this week. Among the 3,185 PIC deaths reported for this week, 2,587 had COVID-19 listed as an underlying or contributing cause of death on the death certificate, and 12 listed influenza, indicating that current PIC mortality is due primarily to COVID-19 and not influenza. The data presented are preliminary and may change as more data are received and processed.
Additional pneumonia, influenza and COVID-19 mortality surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive
Influenza-Associated Pediatric Mortality
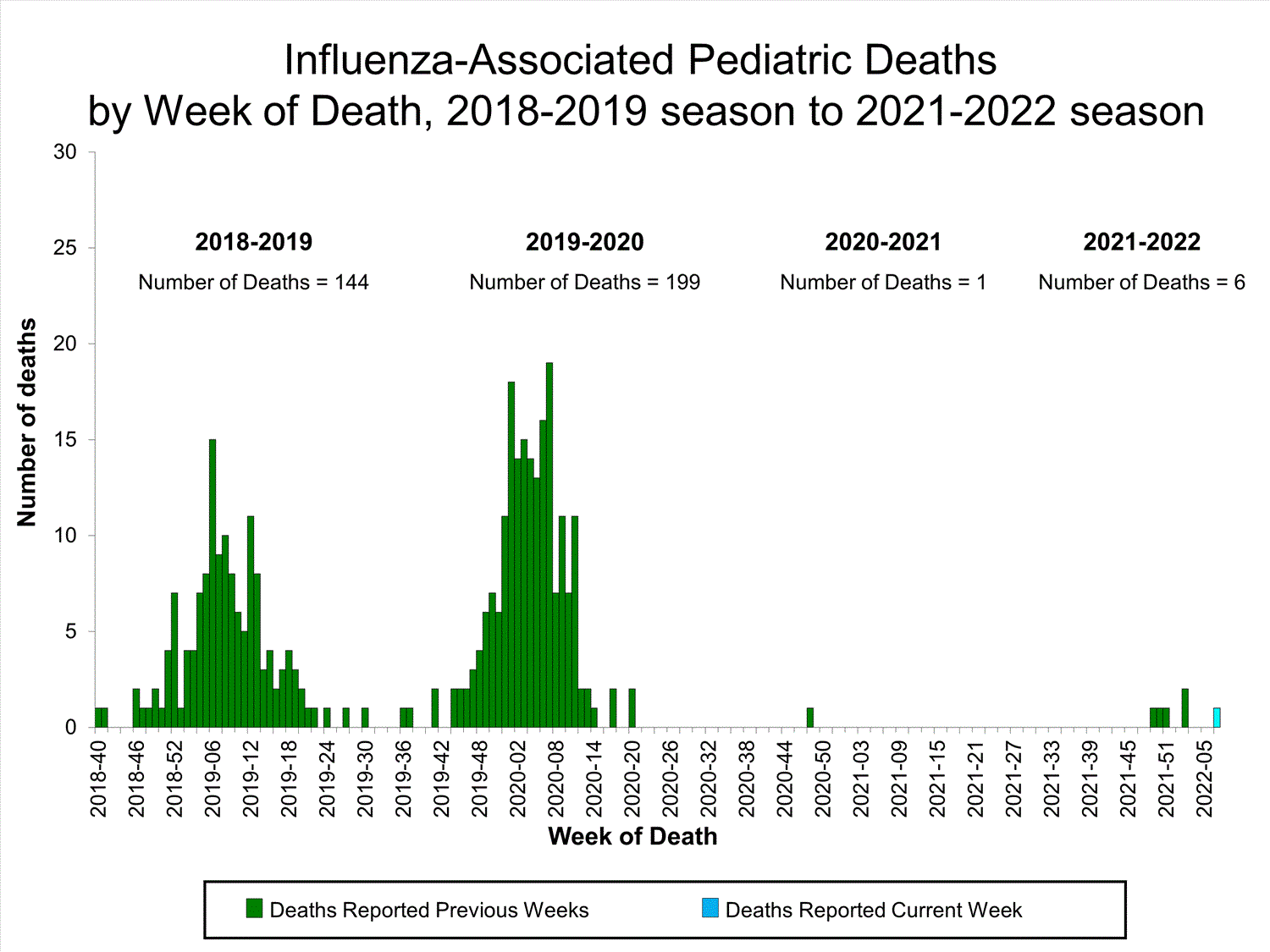
One influenza-associated pediatric death occurring during the 2021-2022 season was reported to CDC during week 7. This death was associated with an influenza A virus for which no subtyping was performed and occurred during week 7.
A total of six influenza-associated pediatric deaths occurring during the 2021-2022 season have been reported to CDC.
Additional pediatric mortality surveillance information for current and past seasons:
Surveillance Methods | FluView Interactive
Additional National and International Influenza Surveillance Information
FluView Interactive: FluView includes enhanced web-based interactive applications that can provide dynamic visuals of the influenza data collected and analyzed by CDC. These FluView Interactive applications allow people to create customized, visual interpretations of influenza data, as well as make comparisons across flu seasons, regions, age groups and a variety of other demographics.
National Institute for Occupational Safety and Health: Monthly surveillance data on the prevalence of health-related workplace absenteeism among full-time workers in the United States are available from NIOSH.
U.S. State and local influenza surveillance: Select a jurisdiction below to access the latest local influenza information.
World Health Organization:
Additional influenza surveillance information from participating WHO member nations is available through
FluNet and the Global Epidemiology Reports.
WHO Collaborating Centers for Influenza:
Australia, China, Japan, the United Kingdom, and the United States (CDC in Atlanta, Georgia)
Europe:
The most up-to-date influenza information from Europe is available from WHO/Europe and the European Centre for Disease Prevention and Control.
Public Health Agency of Canada:
The most up-to-date influenza information from Canada is available in Canada’s weekly FluWatch report.
Public Health England:
The most up-to-date influenza information from the United Kingdom is available from Public Health England.
Any links provided to non-Federal organizations are provided solely as a service to our users. These links do not constitute an endorsement of these organizations or their programs by CDC or the Federal Government, and none should be inferred. CDC is not responsible for the content of the individual organization web pages found at these links.
A description of the CDC influenza surveillance system, including methodology and detailed descriptions of each data component is available on the surveillance methods page.